Post-Herpetic Neuralgia: Understanding and Treating Nerve Pain After Shingles at Peninsula Pain Management
By Dr. James Forbes, Pain Management Specialist – Peninsula Pain Management, New South Wales, Australia
What is Post-Herpetic Neuralgia?
Post-herpetic neuralgia is the most common complication of shingles, caused by damage to the nerves affected by the varicella-zoster virus (the same virus that causes chickenpox). After shingles, some nerves fail to heal properly, leaving them hypersensitive and misfiring pain signals to the brain.
Unlike temporary shingles pain, PHN can last for months or even years, particularly in older adults or those with weakened immune systems.
Brief of Post-Herpetic Neuralgia
As pain specialists, one of the most common and frustrating neuropathic pain conditions we see is post-herpetic neuralgia (PHN). This complication develops in some patients after a shingles outbreak and can cause severe, persistent nerve pain that lingers long after the rash has healed.
While shingles itself is distressing, the burning, stabbing pain of PHN can be life-altering. Patients often describe it as “being on fire,” “needles under the skin,” or “a constant electric shock.” It can disrupt sleep, daily activity, and emotional well-being. Unfortunately, many patients are told they must simply live with the pain.
At Peninsula Pain Management, we know that post-herpetic neuralgia is real, disabling, and treatable. With modern pain management strategies, we can significantly reduce symptoms and help patients regain their quality of life.
Symptoms of Post-Herpetic Neuralgia
Patients with PHN describe symptoms such as:
- Burning or stabbing pain in the area where shingles occurred
- Allodynia: pain from light touch, clothing, or even a breeze
- Hyperalgesia: exaggerated pain from mild stimuli
- Itching, tingling, or numbness in the affected region
- Pain that persists long after the shingles rash resolves
PHN most commonly affects the chest, back, and face (especially around the eye).
Why Does PHN Happen?
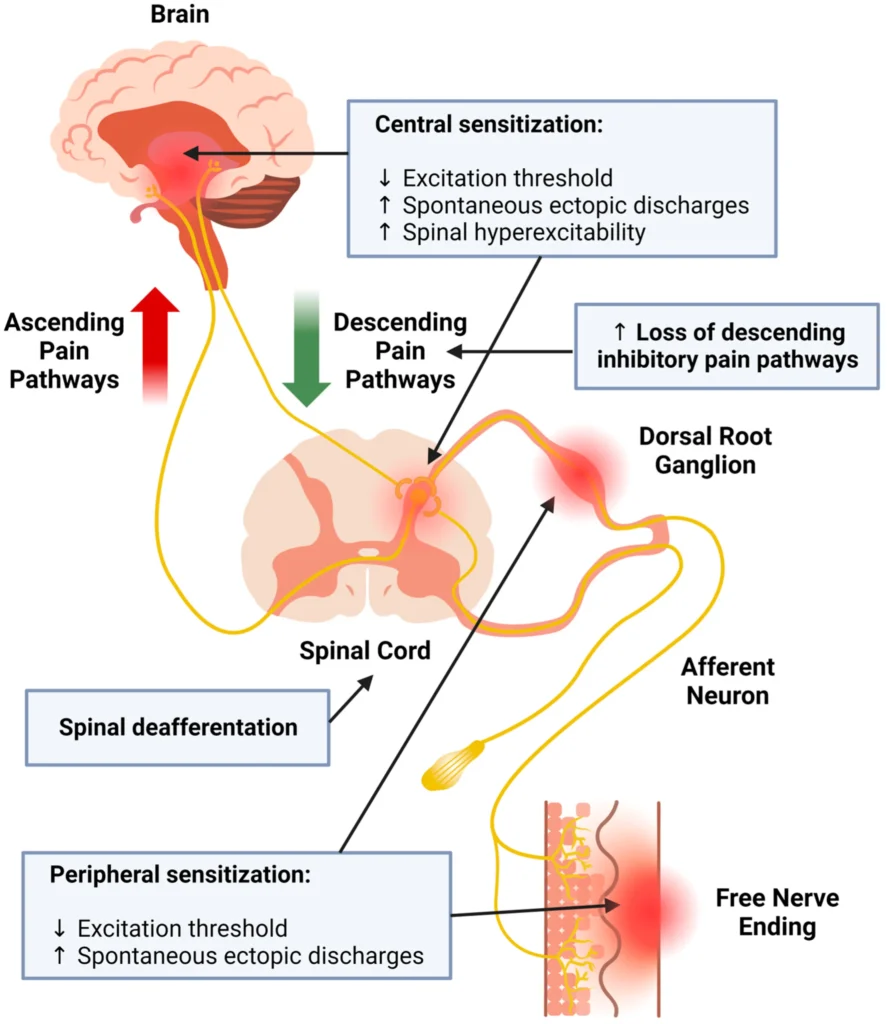
The varicella-zoster virus damages sensory nerves during a shingles outbreak. In some patients, those nerves heal abnormally, becoming hyperexcitable and sending chronic pain signals to the brain.
Risk factors for developing PHN include:
- Age over 60
- Severe shingles rash
- Delayed antiviral
- treatment during shingles
- Weakened immune system
Not everyone develops PHN, but when it does occur, the pain can be severe and long-lasting.
Why Post-Herpetic Neuralgia is Hard to Treat
PHN is a form of neuropathic pain, meaning the problem lies in the nerves themselves—not ongoing infection or inflammation. Standard pain medications like acetaminophen, NSAIDs, or opioids often fail to bring relief.
Instead, patients require specialized therapies that calm nerve activity and retrain the nervous system. At Peninsula Pain Management, we offer exactly these advanced treatments.
How Peninsula Pain Management Treats Post-Herpetic Neuralgia
Our team at Peninsula Pain Management takes a comprehensive, patient-centered approach to treating PHN, combining medications, interventional procedures, and supportive therapies.
Comprehensive Assessment
We begin with a detailed history and physical exam, mapping pain patterns and assessing quality of life. This helps us tailor an individualized treatment plan.
Interventional Pain Management
For patients with severe or medication-resistant PHN, we offer advanced procedures, including:
- Nerve blocks to temporarily interrupt pain signaling
- Epidural steroid injections if inflammation contributes to pain
- Radiofrequency ablation (RFA) for longer-term modulation of nerve activity
- Spinal cord stimulation (SCS), which reprograms pain pathways at the spinal level
- Peripheral nerve stimulation targeting specific areas of persistent PHN
These interventions can dramatically reduce pain intensity and improve quality of life.
Long-Term Support
PHN is a chronic condition for some patients. At Peninsula Pain Management, we provide ongoing care and follow-up, adjusting treatments as needed and supporting patients throughout their journey.
Preventing Post-Herpetic Neuralgia
The best way to reduce the risk of PHN is by preventing shingles itself. Vaccination with the shingles vaccine (Shingrix) is highly effective, especially for adults over 50.
For those who do develop shingles, starting antiviral medication within 72 hours of rash onset can reduce the risk of PHN.
Why Patients Trust Peninsula Pain Management
- Led by Dr. James Forbes, board-certified in pain medicine
- Based in New South Wales, proudly serving the Central Coast
- A reputation for personalised, evidence-based care
- A multidisciplinary approach that puts patient outcomes first
Book Your Appointment
Musculoskeletal pain can affect every part of your life—but you don’t have to face it alone.
Contact Peninsula Pain Management to speak with our team and take the first step toward recovery:
- Phone: [Insert Phone Number]
- Address: [Insert Clinic Address], New South Wales
- Online Booking: [Insert Website or Booking Page]
Medication Management
We use medications proven to target nerve pain, such as:
- Anticonvulsants (gabapentin, pregabalin) to reduce abnormal nerve firing
- Antidepressants (amitriptyline, duloxetine) for neuropathic pain modulation
- Topical lidocaine patches or capsaicin cream for localized relief
- Opioids only in select, carefully managed cases
These medications are used thoughtfully, often in combination, to balance pain relief with minimal side effects.
Non-Pharmacological Therapies
- Physical therapy to maintain mobility and reduce stiffness
- Acupuncture and complementary therapies for some patients
- Cognitive-behavioral therapy (CBT) and mindfulness training to manage the emotional impact of chronic pain
Living with Post-Herpetic Neuralgia
For many patients, post-herpetic neuralgia pain can feel worse than the shingles itself. It can interfere with sleep, personal care, and social activity. Some patients become isolated, anxious, or depressed as the pain persists.
At Peninsula Pain Management, we emphasize that PHN is not “just in your head.” It is a real neurological condition, and effective treatments exist. With the right combination of therapies, most patients can achieve meaningful pain relief and improved daily function.
Peninsula Care
Post-herpetic neuralgia (PHN) is one of the most challenging chronic pain syndromes, but it is not untreatable. At Peninsula Pain Management, we offer a full spectrum of advanced therapies, from nerve-calming medications to interventional procedures such as nerve blocks and spinal cord stimulation. Our mission is to provide lasting relief, restore independence, and improve quality of life for patients living with PHN.
If you or a loved one is struggling with nerve pain after shingles, don’t suffer in silence. At Peninsula Pain Management, expert care and effective treatments are available.


